New analysis of 2020 Financial Health Pulse® data by BlackRock’s Emergency Savings Initiative shows that low- to moderate-income (LMI) frontline workers are less likely to be Financially Healthy than non-frontline workers, a reality that was likely exacerbated by the COVID-19 pandemic. To cope with the financial effects of the pandemic, LMI workers were more likely to draw down their savings and worry about depleting their savings.
On the Front Lines: How LMI Workers Coped During the COVID-19 Pandemic
Key Finding: Low- to moderate-income (LMI) frontline workers are less likely to be Financially Healthy than non-frontline LMI workers.
By Financial Health Network
-
Program:
-
Category:
-
Tags:

LMI Frontline Workers Are Less Financially Healthy Than Non-Frontline Workers
Frontline workers who earn less than $60,000 in household income (LMI) are less likely to be Financially Healthy than other workers at the same household income level who are not frontline workers. In this analysis, we define frontline workers as individuals who came within 6 feet of other people in their jobs regularly (daily, nearly daily, or several times per week) as of August 2020 (see methodology notes for more information). Only 13% of LMI frontline workers are Financially Healthy, compared with 17% of non-frontline workers (see methodology notes for more information). Among those earning less than $60,000, frontline work appears to lower financial health, reducing the likelihood that LMI frontline workers can build financial resilience and pursue opportunities.
Among LMI frontline and non-frontline workers’ financial health, the widest difference was that frontline workers’ incomes were less able to meet their expenses. Over the last year, only 42% of LMI frontline workers were able to spend less than their income, compared with 52% of LMI non-frontline workers. Living paycheck to paycheck left little cushion in workers’ budgets. Among LMI workers, 47% of frontline workers could not pay all their bills on time last year, compared with 38% of non-frontline workers. With bill payments delayed and no income remaining after expenses, LMI frontline workers were vulnerable to emergencies and associated expenses.
The Pandemic Likely Exacerbated Financial Challenges for LMI Frontline Workers
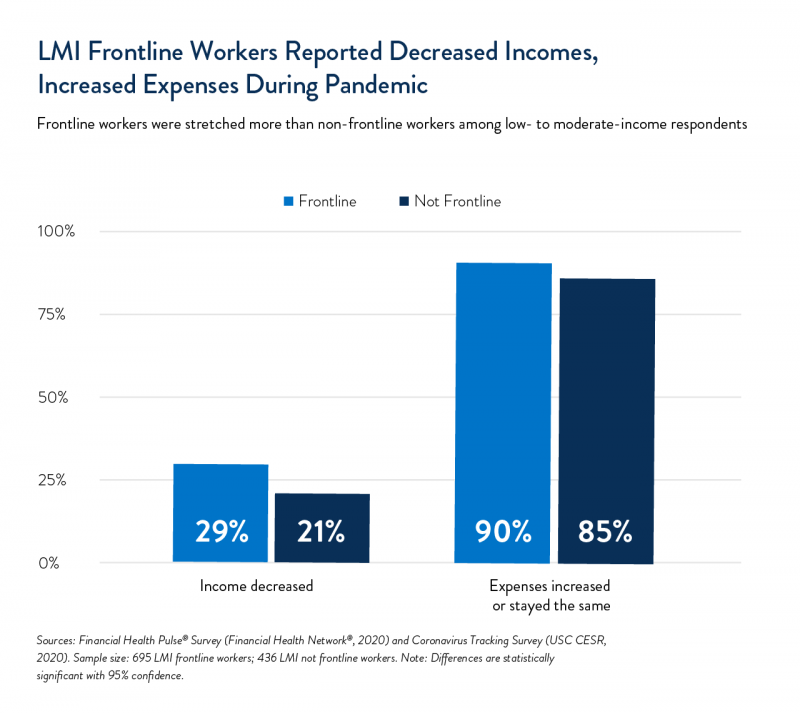
Although we are unable to analyze pre-pandemic comparisons of financial health between LMI frontline and non-frontline workers, we hypothesize that the pandemic may have exacerbated financial health disparities between these groups. During the pandemic, LMI frontline workers were more likely to say their income decreased and their expenses increased or stayed the same. Among LMI frontline workers, 29% reported that their incomes had fallen and 90% reported that their expenses had either increased or stayed the same, compared with 21% and 85% of non-LMI frontline workers, respectively.
Compared with LMI non-frontline workers, LMI frontline workers were more likely to be directly impacted by COVID-19 in their homes and workplaces, affecting both their incomes and expenses. Considering income first, LMI frontline workers were five times more likely (5%) than other LMI workers (1%) to report having someone in their household test positive for COVID-19 at the time of the survey. Beyond the health and emotional well-being effects of this difference, a positive COVID-19 case in the home may have prevented frontline workers from attending work, thus decreasing their income. Further, business closures during the pandemic – caused by frequent policy changes or staff members contracting COVID-19 – led to widespread disruptions in hours and wages for many LMI frontline workers.
Child care challenges during the pandemic also may have affected LMI frontline workers’ income and expenses. LMI frontline workers were more likely to have their work interrupted due to child care responsibilities than other LMI workers. Six percent of LMI frontline workers reported not being able to attend work due to child care and other responsibilities, compared with 1% of LMI non-frontline workers. This time off may have resulted in decreased income, just as child care expenses increased due to school closures and restricted social interactions with family members, who may have provided free child care pre-pandemic.
LMI Frontline Workers Ran Down Their Savings
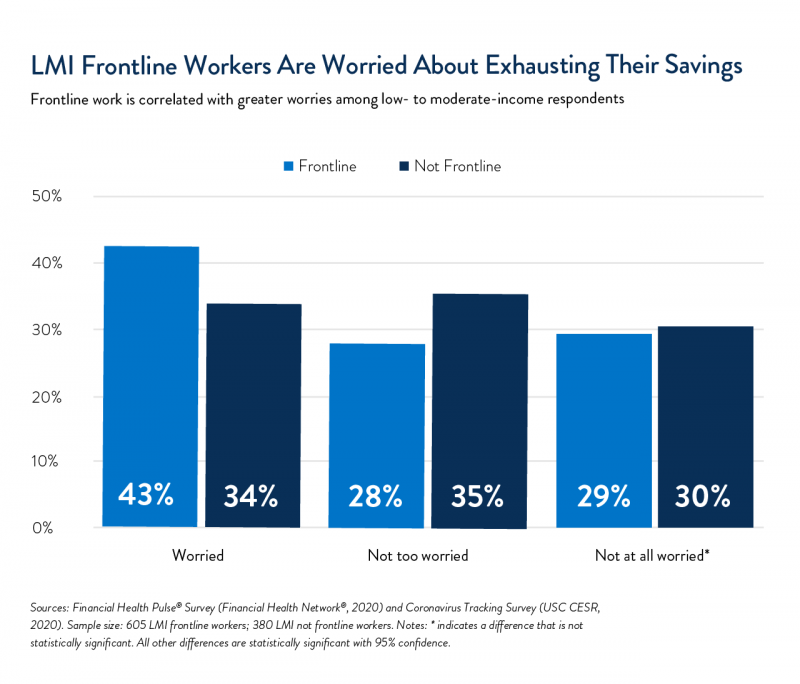
To cope with the financial effects of the pandemic, 29% of LMI frontline workers said they spent down their savings, compared with 23% of other LMI workers. This significant impact reduced the buffer workers had to protect themselves and their households from further emergencies. LMI workers were also more worried about the future: 43% of LMI frontline workers were “worried” or “very worried” that they would exhaust their savings, compared with 34% of LMI non-frontline workers. Despite these challenges, LMI frontline workers are doing their best to save at a similar rate (51%) to their non-frontline counterparts (52%), putting aside money for emergencies.
Solutions Should Focus on Rebuilding Savings and Improving Cash Flow
As we transition to a new economic phase, employers, financial institutions, and policymakers should address the financial health needs of frontline workers by accounting for their variable incomes, greater healthcare risks and child care responsibilities, and diminished savings. Rebuilding emergency savings is a core part of supporting LMI frontline workers’ resiliency as the economy shifts. The private and public sectors have a vital role in supporting LMI frontline workers’ financial health – and providing ways they can access, build, or rebuild savings – during and after the pandemic.
In the workplace, leaders in workers’ financial health are encouraging, supporting, and subsidizing workers’ emergency savings. Offering an emergency savings balance as part of a worker’s total compensation effectively and directly supports workers in building emergency savings; other solutions include savings matching or offering prizes for savings deposits.
Policymakers also have a role in enabling and supporting opportunities for savings innovations through reducing barriers, increasing access, and incentivizing the private sector to address the emergency savings crisis. For financial institutions, focusing on prize-linked savings in small-dollar savings accounts where available has been shown to boost savings activities. Institutions can also increase access to savings accounts by reducing friction in the account opening process.
As employers reflect on the past year, there are opportunities to support LMI frontline workers by building solutions that increase workers’ take-home pay. Increasing wages; building employee emergency or hardship funds; or cutting unavoidable costs, such as healthcare, through improved benefits plans all help to increase workers’ access to income to improve their financial health. These solutions, collectively, would increase LMI frontline workers’ readiness for both regular expenses and emergencies.
Methodology Notes
Data in this report come from two sources: the Financial Health Pulse Survey (July 27 – August 9, 2020) and USC’s Coronavirus Tracking Survey (Wave 10: July 22 – August 18, 2020). These surveys were both fielded to USC’s nationally representative Understanding America Panel (UAS), allowing us to join the responses of individuals who participated in both. The final sample included in this analysis was 1,751 individuals over 18 years old who are classified as LMI workers with less than $60,000 in annual household income. In this analysis, we define frontline workers as individuals who come within 6 feet of other people in their jobs regularly (daily, nearly daily, or several times per week). Financial health was measured according to the Financial Health Network’s FinHealth Score® methodology.
This emergency savings analysis was completed in partnership with Blackrock’s Emergency Savings Initiative
![]()
Our Supporters
The Financial Health Pulse is supported by the Citi Foundation. Since the inception of the initiative in 2018, the Financial Health Network has collaborated with USC’s Dornsife Center for Economic and Social Research (CESR) to field the study to their online panel, the Understanding America Study. Study participants who agree to share their transactional and account data use Plaid’s data connectivity services to authorize their data for analysis.
The findings, interpretations, and conclusions expressed in this piece are those of the Financial Health Network and do not necessarily represent those of our funders or partners.


